Private: How to Increase Patient Collections Before 2022

The rise in healthcare costs over the past few years has impacted both patients and providers alike. Consumers are choosing higher deductibles to secure lower monthly premiums, leading to larger medical bills and declining patient collections. Deductibles for single workers have increased 54 percent over the past five years, while out-of-pocket costs have increased by 4.6% percent in 2019. As patients struggle to cover ever-growing medical expenses, providers are finding it harder to collect unpaid bills. Patient collection rates must increase if practitioners want to avoid potentially crippling losses.
Studies show that 62 percent of healthcare providers’ administration costs are spent on billing and insurance-related activities. If collection rates were higher, this number would not be as concerning. However, with 36 percent of hospitals reporting $10 million of bad debt in 2018, providers are looking for more efficient methods of recovering patient collections. Outsourcing certain administrative duties to third-party vendors may help lower these costs and improve collection rates.
Benefits of Using a Third-Party Vendor for Patient Collections
Practitioners do not have time to create these systems, and nor should they. The focus of a healthcare provider and its staff should be on treatment and customer service. A study conducted by Public Agenda in 2017 revealed that only 23 percent of adults received information on payment options and costs from their healthcare provider. Although staff members are encouraged to discuss all aspects of care with consumers, enlisting a third-party vendor to inform each patient of his or her payment options takes the burden off of busy employees.
Administrative Cost Reduction

Hiring in-house staff to oversee billing is not always the most cost-effective solution for providers. Time spent processing patient payments and chasing unpaid invoices keeps employees from addressing more urgent issues faced by consumers. Outsourcing billing services means providers can save money they otherwise spend on full- or part-time salaries for in-house employees. Training costs are also reduced as staff is free to address more pressing matters instead of learning new billing protocols.
Reduction in Human Error
Healthcare workers may be asked to liaise with various departments, out-of-network offices, and large insurance companies to file one claim. If not communicated correctly, errors in the submission paperwork or billing codes may occur, leading to further delays in collection. Third-party billing systems use smart technology to scan claims for consistency and accuracy, essentially eliminating the probability of human error. Fewer errors translate to fewer rejected claims and faster reimbursements.
Billing Security

The Covid-19 Pandemic severely heightened healthcare cybersecurity threats over the last year. In fact, 93 percent of healthcare organizations have experienced a data breach over the past three years, while 57 percent have had more than five data breaches during this time. The security of a patient’s records, billing information, and claim data is paramount to building trust between the provider and the consumer. Only select third-party billing companies are HITRUST CSF certified, protecting both the provider and patient against data breaches. By offering services with heightened security measures, third-party vendors gain trust from the patient, which in turn benefits the provider.
3 Ways Third-Party Billing Services Increase Patient Collections
Healthcare providers often use a combination of multiple systems that manage patients’ records, billing information, insurance details, and claim history. Overworked employees searching these systems for sensitive data may generate conflicting or inaccurate information. As a result, patients may become unclear on their financial responsibility and reject unexplained medical bills. Third-party billing services have the time and resources to create streamlined systems that work for both the provider and the patient.
1. Consistent Billing Design
A clearer billing design helps consumers better understand their financial responsibility and the payment options available to them. Third-party vendors have the expertise to create user-friendly bills that draw on key tendencies in human behavior. For example, consistency in design translates to familiarity. If a patient becomes familiar with the bill’s design and intent, he or she may be more inclined to trust the source and pay on time.
Taking advantage of color-printed billing statement options is another simple way to ensure your medical bill effectively communicates responsibility to patients. In fact, 54 percent of people are more likely to read a document printed in color, and 43 percent of people were more likely to pay a bill on time if the statement is in color. Color-printed statements can keep your customers more engaged in your company and save significant capital that would otherwise be spent on duplicate mailings and late statements.
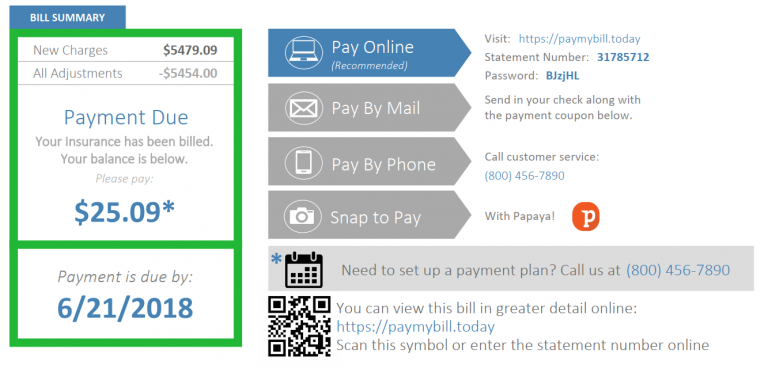
2. Improved Patient Payments
Consumers are often looking for the easiest way to pay bills and keep track of their finances. Advanced third-party billing services offer a variety of digital and traditional payment methods that providers do not have the infrastructure or time to create and maintain. Patient payments through third-party systems can be made with smartphones via text message, online portals, or by scanning a QR code within seconds, from any location. Presenting consumers with the choice to pay instantly through mobile devices may help increase patient collections otherwise delayed through the mail. In the case of MailMyStatement’s patient payment options, the software is protected by the prestigious HITRUST certification, ensuring heightened security for your sensitive patient health information.
Online Portals
Online portals allow patients to view their entire billing history in one place, leading to a greater awareness of their financial responsibility. A study conducted by TransUnion Analysis found that 90 percent of providers still use paper and manual systems for patient collections. Outsourcing the process to companies that use the latest technology in online billing software may help providers collect funds faster.
Pro Tip: MailMyStatements’ EasyAdmin portal allows clients to manage all patient billing and payment functions through one simple interface. Patients also receive access to this portal where they are able to opt-in and out of different billing communication options like paper, estatement, or text alert.
Payment Plans
A recent study conducted by Kaiser Health revealed that 67 percent of patients are concerned about surprise bills. Receiving excessive or unexpected bills can be devastating for consumers without financial safety nets. The same study noted that 40 percent of insured adults received unexpected bills in the space of one year. Offering payment plans to consumers may help providers collect the full amount owed without having to continually chase patients struggling with high out-of-pocket costs.

3. One Integrated System
Third-party vendors often use advanced technologies that integrate seamlessly with existing networks used at healthcare institutions. Navigating multiple services across various departments to collect patient information may cause staff to miss important deadlines or create errors in billing. A system that integrates with all existing services means hospitals do not need to update their own protocols or install new ones.
Recent reports suggest that healthcare providers are seeing an improvement in their collections by enlisting third-party vendors to manage administrative duties. These results imply that outsourcing can lead to lower costs, provide better services for the patient, and create a more streamlined workflow for staff members. As healthcare costs continue to rise, third-party billing services may be the best method of increasing patient collection rates and avoiding bad debt.
Position your healthcare system to start off 2022 on a high note with increased revenues. MailMyStatements offers a variety of simplified billing systems ranging from intelligent statement design to technology-driven payment options. Let’s get in touch and discuss if our solutions may be a good fit for your healthcare system.
LEARN MORE ABOUT HOW OUR SOLUTIONS CAN SAVE YOU TIME AND MONEY!

Michael Bell is the Chief Marketing Officer for MailMyStatements. Mike is a dynamic, innovative thinker, a healthcare technology advocate, a consumer, a patient, and an avid golfer.
Follow him on Twitter!
@staroneconsult
![]()



